From Loss Runs to Risk Intelligence.
Extract every claim from any carrier PDF, DOCX, or Excel, surface it on a live dashboard grouped by client, and turn it all into a renewal-ready AI loss summary in one click
Extract every claim, every field.
PDF, DOC/DOCX, XLS/XLSX, carrier-formatted, broker-formatted, or scanned. Up to 20 documents at a time. Carrier, policy number, claim ID, claimant, paid, reserve, recovery, net incurred, deductible billed, captured and normalized out of the box, plus any custom field your schema defines.
Extract every claim, every field.
PDF, DOC/DOCX, XLS/XLSX, carrier-formatted, broker-formatted, or scanned. Up to 20 documents at a time. Carrier, policy number, claim ID, claimant, paid, reserve, recovery, net incurred, deductible billed, captured and normalized out of the box, plus any custom field your schema defines.
Live claims reporting.
Use the live filterable claims table, generate loss summary reports to identify key trends or anomalies, and export loss data in client-ready Excel reports. All built for the way claims actually get reviewed.
Live claims reporting.
Use the live filterable claims table, generate loss summary reports to identify key trends or anomalies, and export loss data in client-ready Excel reports. All built for the way claims actually get reviewed.
Made for easy review.
Every claim links back to its source in the original document. Open the extraction, see the source page side-by-side, and quickly review any potential issues that have been flagged - so QA takes minutes, not hours.
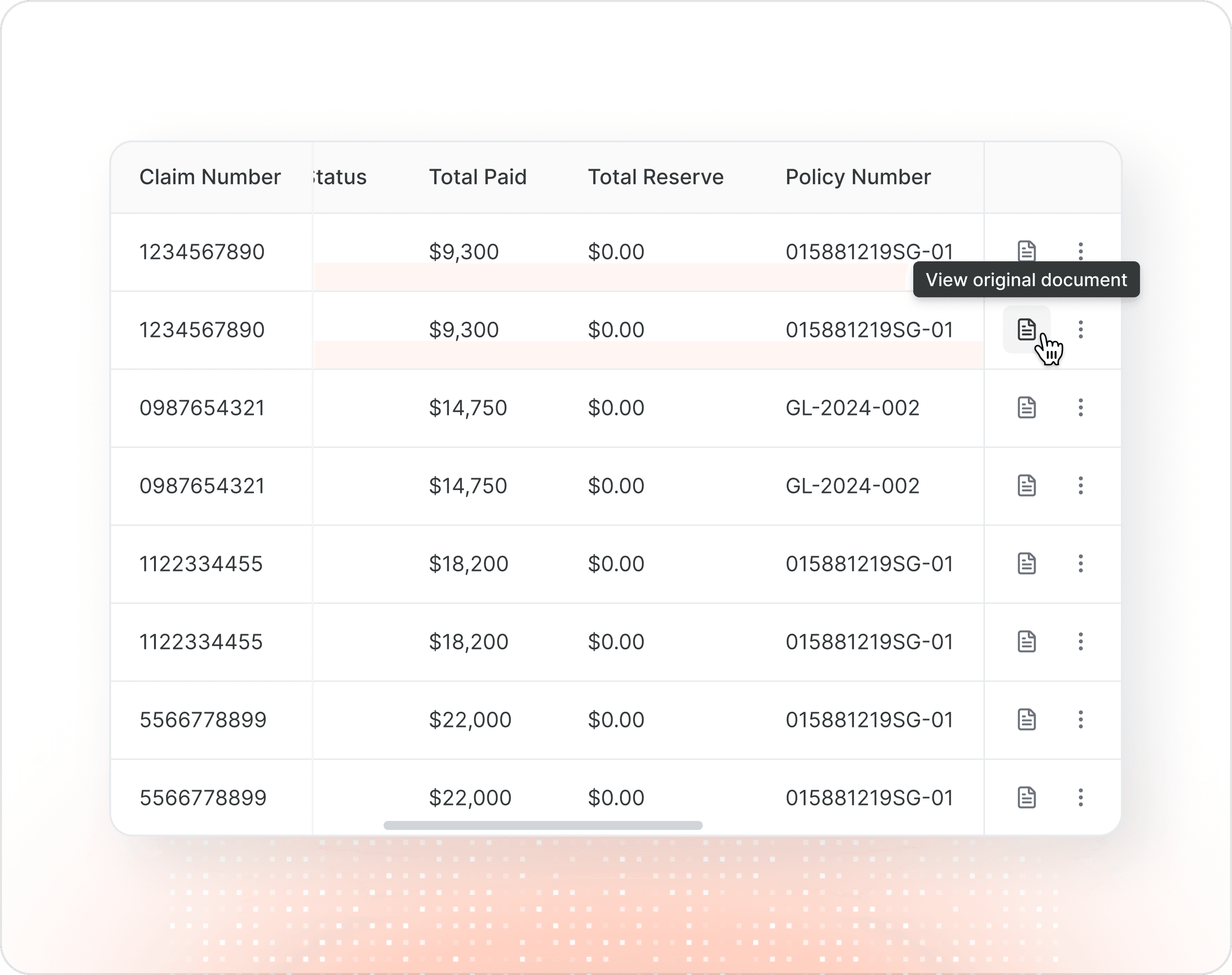
Made for easy review.
Every claim links back to its source in the original document. Open the extraction, see the source page side-by-side, and quickly review any potential issues that have been flagged - so QA takes minutes, not hours.

Ask anything. Summarize everything.
Chat directly with your loss runs to dig into specific claims, or generate a complete AI-written loss summary for renewal in one click, covering trends, severity outliers, and the red flags carriers care about most.
Ask anything. Summarize everything.
Chat directly with your loss runs to dig into specific claims, or generate a complete AI-written loss summary for renewal in one click, covering trends, severity outliers, and the red flags carriers care about most.
Auto-load into your analytics pipeline.
Extracted claims flow straight into your data warehouse and analytics dashboards, fueling trend reports, retention models, and renewal forecasting without a separate data engineering project.
Auto-load into your analytics pipeline.
Extracted claims flow straight into your data warehouse and analytics dashboards, fueling trend reports, retention models, and renewal forecasting without a separate data engineering project.
Common questions
What documents can I upload?
PDF, DOC/DOCX, and XLS/XLSX loss runs, up to 20 at a time. Carrier-formatted, broker-formatted, or scanned, we handle all of them.
What does it actually extract?
Carrier, policy number, policy period, product line, claim ID, claim status, claimant, paid, reserve, recovery, net incurred, and deductible billed, out of the box. Plus any custom field your schema defines.
Can I trust the numbers?
Every claim links back to its source document. Open the extraction, see the original page side-by-side, re-run validation in one click.
Do you order loss runs from carriers too?
Yes. Loss Runs Pro orders, tracks, and manages loss-run requests across your entire book. When the carrier delivers, extraction runs automatically.
What’s the output?
A live claims dashboard, a filterable claims table, an AI-generated claims summary, and downloadable Excel reports, single-doc or merged across many. Plus auto-load into your analytics pipeline for trend reporting.
Common questions
What documents can I upload?
PDF, DOC/DOCX, and XLS/XLSX loss runs, up to 20 at a time. Carrier-formatted, broker-formatted, or scanned, we handle all of them.
What does it actually extract?
Carrier, policy number, policy period, product line, claim ID, claim status, claimant, paid, reserve, recovery, net incurred, and deductible billed, out of the box. Plus any custom field your schema defines.
Can I trust the numbers?
Every claim links back to its source document. Open the extraction, see the original page side-by-side, re-run validation in one click.
Do you order loss runs from carriers too?
Yes. Loss Runs Pro orders, tracks, and manages loss-run requests across your entire book. When the carrier delivers, extraction runs automatically.
What’s the output?
A live claims dashboard, a filterable claims table, an AI-generated claims summary, and downloadable Excel reports, single-doc or merged across many. Plus auto-load into your analytics pipeline for trend reporting.
Common questions
What documents can I upload?
PDF, DOC/DOCX, and XLS/XLSX loss runs, up to 20 at a time. Carrier-formatted, broker-formatted, or scanned, we handle all of them.
What does it actually extract?
Carrier, policy number, policy period, product line, claim ID, claim status, claimant, paid, reserve, recovery, net incurred, and deductible billed, out of the box. Plus any custom field your schema defines.
Can I trust the numbers?
Every claim links back to its source document. Open the extraction, see the original page side-by-side, re-run validation in one click.
Do you order loss runs from carriers too?
Yes. Loss Runs Pro orders, tracks, and manages loss-run requests across your entire book. When the carrier delivers, extraction runs automatically.
What’s the output?
A live claims dashboard, a filterable claims table, an AI-generated claims summary, and downloadable Excel reports, single-doc or merged across many. Plus auto-load into your analytics pipeline for trend reporting.

Ready to Transform Your Agency?

Ready to Transform Your Agency?

Ready to Transform Your Agency?
The #1 AI platform for insurance. 250+ agencies. Purpose-built workflows. Enterprise security.
The #1 AI platform for insurance. 250+ agencies. Purpose-built workflows. Enterprise security.
The #1 AI platform for insurance. 250+ agencies. Purpose-built workflows. Enterprise security.
Platform